Table of Contents
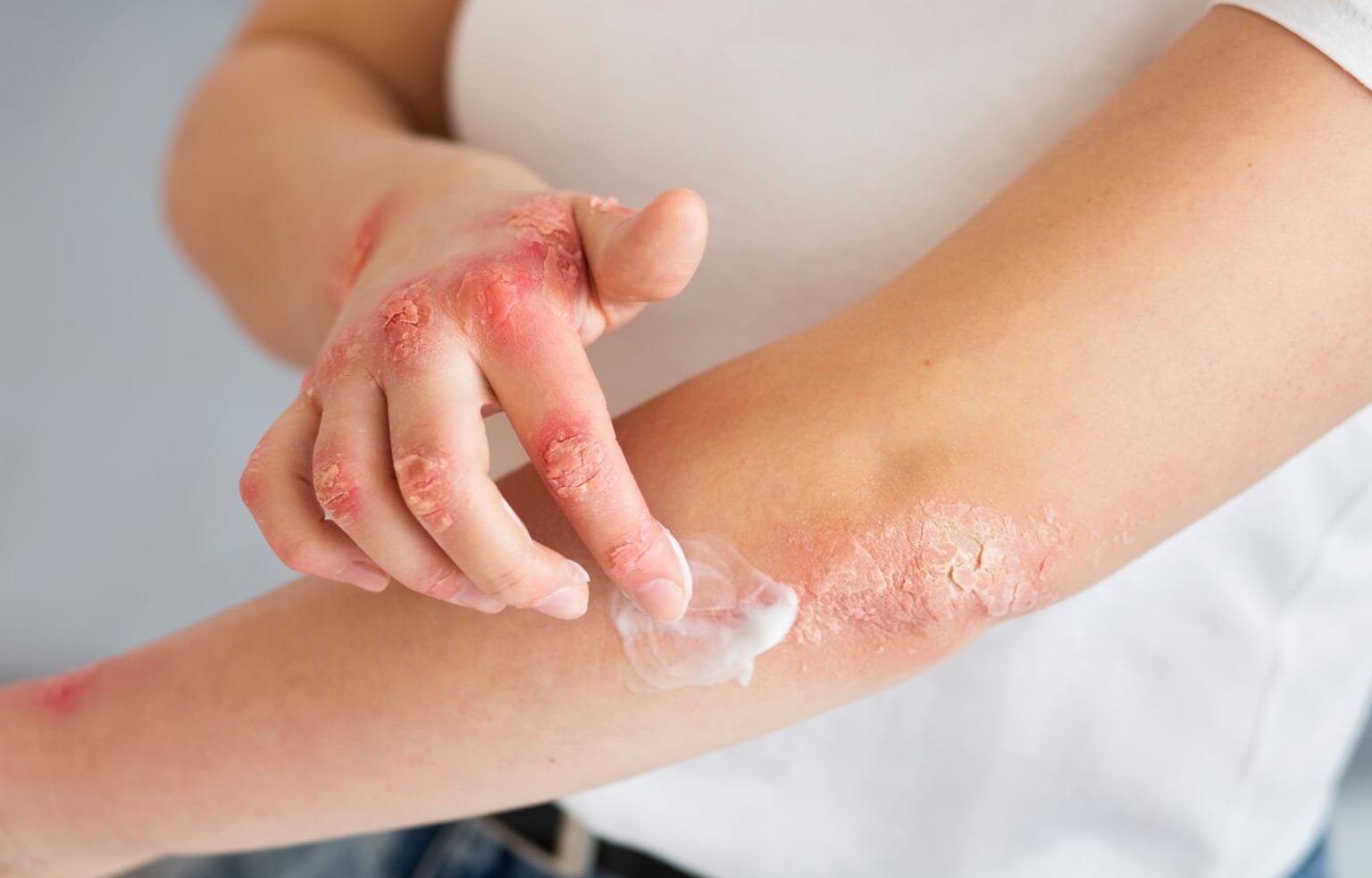
Functional medicine is transforming the way we approach chronic health conditions and autoimmune disorders. By focusing on the root causes of illness and supporting the body’s natural healing processes, functional medicine offers a personalized path to better health. One of the cornerstones of this approach is the strategic use of high-quality supplements.
At Hormone Reset, India’s leading functional medicine clinic, we guide patients toward evidence-based supplement choices that are tailored to their unique needs. In this blog, we’ll explore the top-rated functional medicine supplements that support chronic disease recovery and optimal wellness.
What Is Functional Medicine?
Functional medicine is a patient-centered, science-based approach that looks beyond symptoms to identify and address the underlying causes of disease. Unlike conventional medicine, which often focuses on symptom management, functional medicine uses a holistic framework to understand how genetics, environment, and lifestyle factors contribute to chronic illness. Supplements play a key role in functional medicine by correcting key nutrient deficiencies, supporting biochemical pathways, and enhancing the body’s ability to heal.
Why Supplements Matter in Functional Medicine
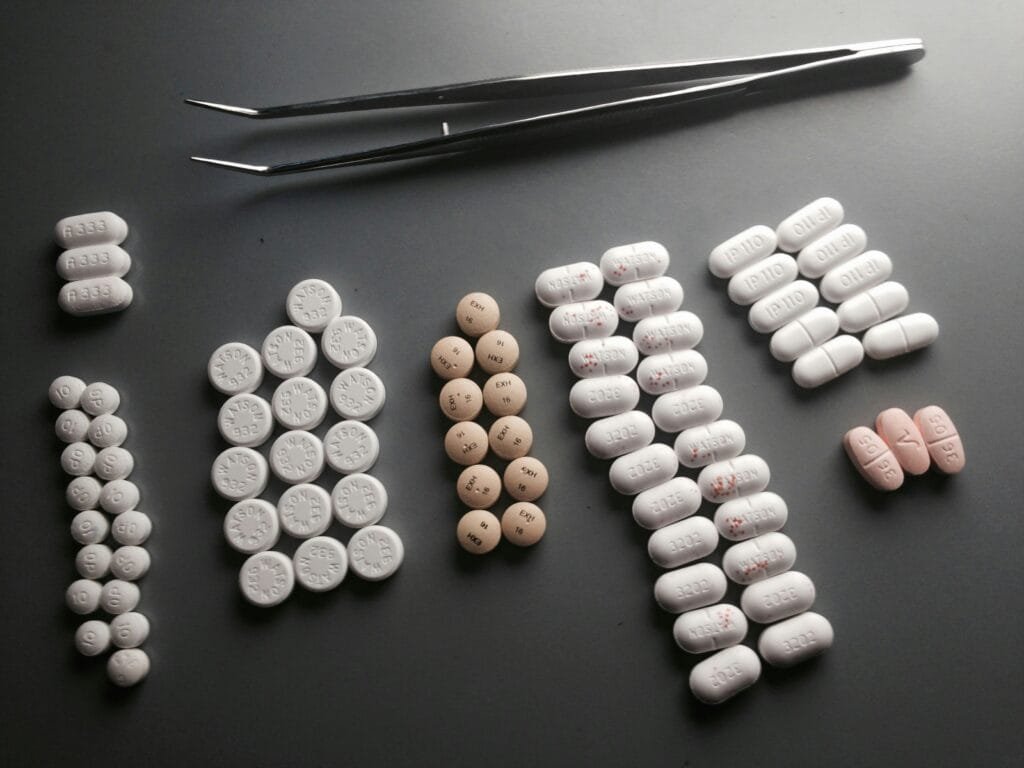
Many chronic and autoimmune conditions are linked to nutrient deficiencies, inflammation, and imbalances in gut health. Supplements, when chosen wisely, can fill nutritional gaps, modulate inflammation, and restore balance. For example, research shows that patients with chronic conditions often lack essential nutrients like the B vitamins, vitamin D, magnesium, and omega-3 fatty acids. Adding these nutrients often improves their health significantly. Functional medicine supplements are selected based on individual needs, lab testing, and current scientific evidence—ensuring maximum safety and effectiveness.

5 Essential Supplements Recommended in Functional Medicine
Omega-3 fatty acids are vital for reducing inflammation, supporting cardiovascular health, and enhancing immune function. EPA and DHA, the biologically active forms of omega-3 fatty acids, help regulate inflammatory pathways, optimize cellular communication, and support cognitive function. Functional medicine research shows that people with autoimmune conditions, metabolic syndrome, or chronic inflammatory disorders often have low omega-3 levels, which can exacerbate disease activity. Incorporating omega-3s through dietary sources such as fatty fish or through supplements has been shown to reduce markers of inflammation, improve lipid profiles, and support overall wellness.
Recommendation: Vitaone Triple Strength Omega 3, 60 Soft Gels, Autoimmunity Care Vegan Omega 3 Oil, 250 ML
Probiotics are essential for maintaining a healthy gut microbiome, which plays a central role in digestion, nutrient absorption, immune regulation, and even mental health. A well-balanced microbiome strengthens the intestinal barrier, reduces systemic inflammation, and modulates immune responses. Disruptions due to antibiotics, stress, processed foods, or poor diet can lead to dysbiosis, contributing to digestive discomfort, fatigue, and chronic inflammation. Clinical studies highlight the benefits of multi-strain probiotics containing Lactobacillus and Bifidobacterium in restoring gut balance, enhancing nutrient absorption, and supporting immune resilience.
Recommendation: FM Nutrition Opti-Biotic, Multi-strain Probiotics, 100 billion CFU, 60 Veg Capsules
Vitamin D3 functions as both a vitamin and hormone, playing a critical role in immune modulation, bone health, and inflammatory control. Research indicates that vitamin D deficiency is widespread in India, due to limited sun exposure, high melanin content, indoor lifestyles, and environmental factors. Low vitamin D levels are associated with increased risk of autoimmune diseases, impaired bone density, and chronic inflammation. Functional medicine protocols emphasize testing serum vitamin D levels and tailoring supplementation to individual needs to optimize immune function, reduce inflammation, and support musculoskeletal health.
Recommendation: Vitaone Vitamin D3 + K2-7, 90 Veg, Dr Gold Vitamin D3K2 I 60 Capsules
Magnesium is a cofactor in over 300 enzymatic reactions and is essential for energy production, muscle relaxation, nerve signaling, stress management, and sleep quality. Modern diets, soil depletion, chronic stress, gastrointestinal disorders, and certain medications often lead to suboptimal magnesium levels. Clinical studies demonstrate that magnesium supplementation can alleviate muscle cramps, improve sleep patterns, reduce anxiety symptoms, and enhance cardiovascular health. Functional medicine practitioners recommend bioavailable forms such as magnesium glycinate or citrate to maximize absorption and physiological benefit.
Recommendation: LivBio SuperMag Plus, Magnesium Supplement, 30 Veg Capsules
Coenzyme Q10 (CoQ10) is a lipid-soluble antioxidant that plays a key role in mitochondrial energy production. It supports cardiovascular function, muscle performance, and neurological health by facilitating cellular ATP synthesis. CoQ10 levels naturally decline with age and can be further depleted by chronic illness, oxidative stress, or medications such as statins. Clinical studies highlight that CoQ10 supplementation may improve energy metabolism, reduce fatigue, enhance exercise tolerance, and protect cells from oxidative damage, making it a cornerstone in functional medicine protocols for cellular health and longevity.
Recommendation: FM Nutrition Liposomal CoQ10, Ubiquinol 200mg, 30 Veg Capsules
How to Choose the Right Supplements for You
Supplementation should always be personalized. Functional medicine practitioners at Hormone Reset use detailed health histories, lab testing, and ongoing monitoring to create individualized supplement protocols. Avoid self-prescribing, as taking the wrong supplements or incorrect dosages can be harmful. Professional guidance ensures that supplements are safe, effective, and aligned with your health goals.
Frequently Asked Questions About Functional Medicine Supplements
Are supplements safe for everyone?
Most supplements are safe when used appropriately, but some may interact with medications or underlying health conditions. Always consult a qualified practitioner.
How long before you see results?
Some supplements work quickly (e.g., magnesium for muscle cramps), while others may take longer to show benefits. Consistency and professional monitoring are key.
Can supplements replace medication?
Supplements can support healing but should not replace prescribed medications without medical supervision. Functional medicine integrates supplements with other therapies for comprehensive care.
Conclusion
Functional medicine supplements offer a powerful way to support healing, restore balance, and address the root causes of chronic and autoimmune disorders. At Hormone Reset, we combine expert guidance with evidence-based protocols to help you achieve optimal health. Ready to take the next step? Schedule a consultation with our functional medicine experts and discover a personalized path to wellness.
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before starting any new supplement regimen.
References
- The role of probiotic supplementation in inflammatory biomarkers in adults– National Library of Medicine
- Prevalence & potential significance of vitamin D deficiency in Asian Indians– Indian Journal of Medical Research
- Why You Should Consider Taking Omega-3 Supplements– NDTV
- Make no bones about it! Vitamin D deficiency a major worry, every 5th Indian suffers from it– Times of India
- The effects of coenzyme Q10 supplementation on biomarkers of exercise-induced muscle damage, physical performance, and oxidative stress– National Library of Medicine
- The effect of omega-3 and vitamin E on oxidative stress and inflammation– National Library of Medicine
Please subscribe to our social channels for updates related to functional medicines.
Instagram: thehormonereset
Facebook: Hormone Reset
YouTube: Hormone Reset Program
LinkedIn: Hormone Reset