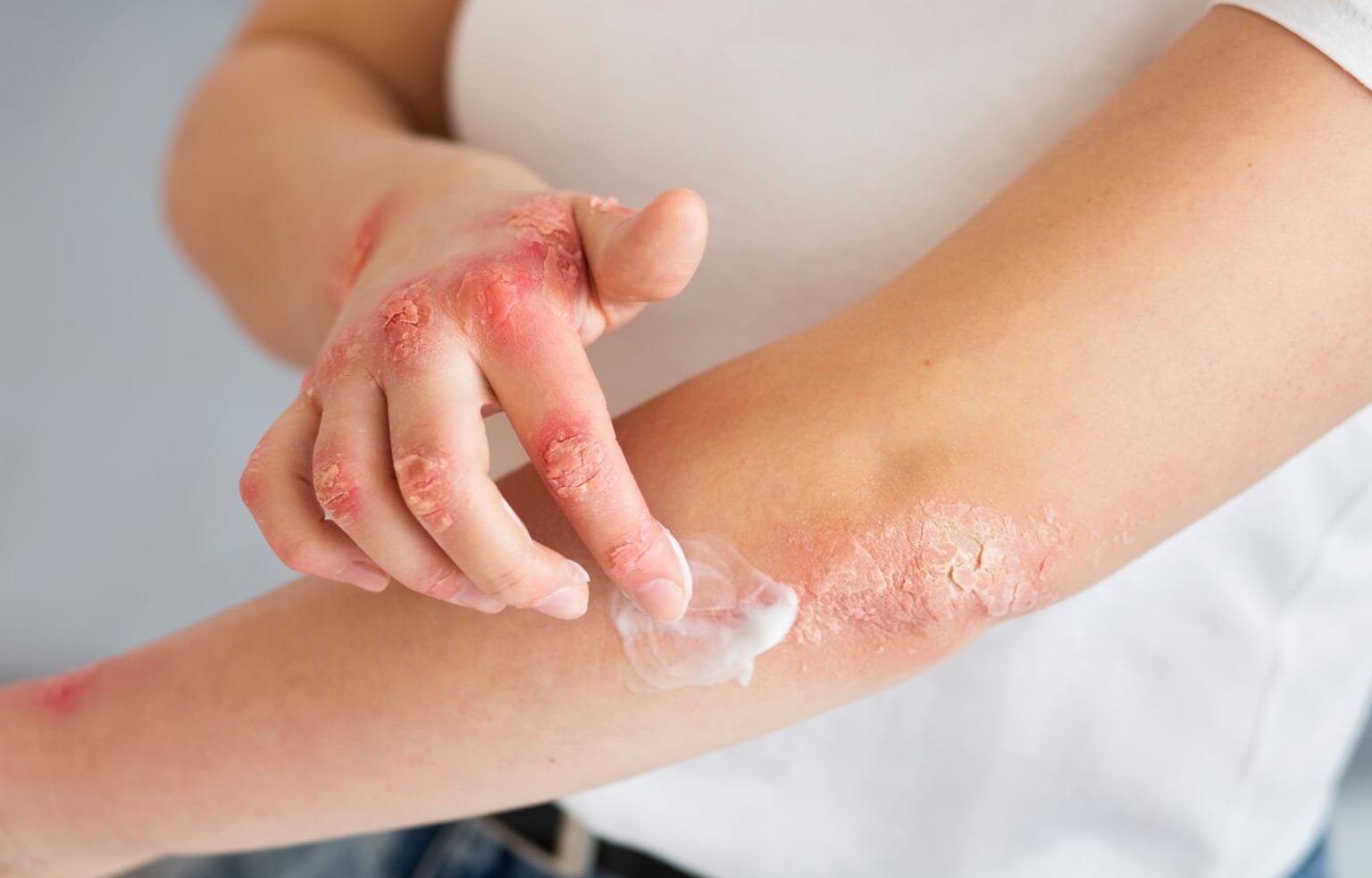
Lichen Planus resulting in mysterious itchy, purplish rashes? Mouth sores that sting when you eat spicy foods? Or white lacy patches on your gums or inner cheeks? You might be dealing with a little-known autoimmune condition called Lichen planus.
And here’s the truth: lichen planus isn’t just skin-deep. It’s a reflection of what’s going on inside your body, specifically, with your immune system and your hormones.
At Hormone Reset, we go beyond the surface. We don’t just treat symptoms — we decode the root causes. And when it comes to autoimmune disorders like lichen planus, our Functional Medicine Approach has helped hundreds rediscover glowing skin, healthy immunity, and internal balance.
What Is Lichen Planus?
Lichen planus is a chronic, inflammatory, autoimmune condition where your immune system mistakenly attacks the body’s own tissues — especially the skin and mucous membranes. It’s more common than people think and can be extremely uncomfortable and persistent if not properly diagnosed and treated.
This condition can appear suddenly or gradually, and the symptoms often fluctuate with changes in hormone levels, stress, and inflammation. While it’s not contagious or cancerous, it can cause significant distress and affect daily life.
Common Areas Affected:
- Skin: Purple, flat-topped, itchy bumps often grouped in patches. These bumps can leave dark marks or scarring even after healing.
- Mouth: White, lacy patches or painful ulcers that affect the inside of cheeks, gums, tongue, and lips, making it hard to eat or talk.
- Scalp: Inflammation in hair follicles leading to redness, itching, and eventually permanent hair loss, also known as lichen planopilaris.
- Nails: Thinning, ridging, grooving, or in severe cases, complete nail loss, often mistaken for fungal infections.
- Genitals: Painful erosions, redness, and discomfort, which can interfere with intimacy and emotional wellbeing.
Symptoms to Watch For:
- Intense itching or burning sensations, especially on the wrists, ankles, or lower back.
- Painful eating or speaking due to oral sores that worsen with spicy or acidic foods.
- Changes in nail or hair texture that don’t improve with standard treatments.
- Fatigue and emotional stress that seem to coincide with flare-ups.
- Symptoms often flare during hormonal transitions such as menstruation, pregnancy, or menopause.
What Triggers Lichen Planus?
- Hormonal imbalance, such as thyroid issues or fluctuating estrogen levels, which may worsen immune reactivity.
- Chronic stress and trauma, both physical and emotional, that weaken immune and hormonal regulation.
- Leaky gut and microbiome imbalance, which activate inflammatory pathways.
- Medications, including NSAIDs, beta-blockers, and certain vaccines that may act as triggers.
- Heavy metal exposure or dental fillings, which can overstimulate the immune system.
- Hepatitis C and viral infections, strongly associated with oral and cutaneous lichen planus.
- Food sensitivities or allergies, especially to gluten, dairy, and artificial additives.
Also Read: Living with Multiple Autoimmune Condition
Why Conventional Medicine Often Misses the Mark?

Most conventional treatments aim to suppress symptoms using medications like corticosteroids, antihistamines, and immunosuppressants. These may temporarily ease the rash or pain but don’t address the root cause.
Patients often cycle through various treatments with limited results. Long-term use of these medications can damage the skin, disrupt gut health, and impair hormone balance, sometimes making the condition worse over time.
Autoimmunity is a full-body issue — and it needs a full-body solution that restores balance, not just suppresses the body’s signals.
The Functional Medicine Perspective: Healing From the Inside Out
At Hormone Reset, we believe the body is designed to heal — when given the right support and environment. Functional medicine focuses on uncovering the root causes of disease and customizing healing plans based on your biology.
We focus on understanding how your hormonal, digestive, detoxification, immune, and nervous systems work together — and where they might be out of balance.
1. Comprehensive Root Cause Testing
We begin by assessing your whole system with advanced functional labs that uncover hidden imbalances. These tests provide a detailed picture of what’s driving your symptoms.
- Hormone Panels assess thyroid, adrenal, and sex hormone levels to identify imbalances like low T3 or estrogen dominance. These imbalances often fuel immune dysfunction and skin flare-ups.
- Inflammation Markers like CRP and ESR reveal ongoing immune activity that standard tests may miss. Elevated levels signal underlying inflammation driving lichen planus.
- Micronutrient Testing uncovers deficiencies that impact immune repair and detoxification. Key nutrients like zinc, vitamin D, and B-complex vitamins are essential for tissue healing.
- Gut Microbiome & Stool Analysis detects hidden infections, leaky gut, and poor digestion. An unhealthy gut contributes to autoimmune flare-ups through immune system confusion.
- Toxin Screening identifies heavy metals, mold exposure, and chemical toxicity contributing to inflammation. Reducing toxic burden can help calm the immune system.
These tests help uncover silent root causes that standard medical testing often overlooks.
2. Hormone Rebalancing
Hormones regulate immunity, stress responses, and tissue repair. When they are out of sync, autoimmunity can flare.
We assess hormone patterns and use natural therapies to restore balance. This includes herbal adaptogens, seed cycling, personalized nutrition, and where needed, bioidentical hormone support to stabilize hormonal rhythms and reduce immune overactivity.
Our strategies target the root hormonal disruptions behind inflammation and skin flare-ups.
3. Immune Reset Through Gut Healing
Gut health is central to immune health. An imbalanced gut can allow harmful particles to enter the bloodstream, triggering immune confusion and attacks on healthy tissue.
We restore gut integrity through food eliminations, healing supplements like L-glutamine and collagen, and microbiome restoration using high-quality probiotics and herbs that rebalance gut flora.
When the gut heals, the immune system calms down and stops attacking your tissues.
4. Detox Pathway Activation
A sluggish detox system means toxins accumulate and trigger inflammation. We support your body’s natural detox organs so they can clear irritants that fuel autoimmune reactions.
This includes gentle herbal cleanses, supporting liver enzymes, increasing hydration with mineralized water, and avoiding daily toxin exposures like plastics, pesticides, and synthetic fragrances.
When detox pathways are supported, skin and immune symptoms improve significantly.
5. Nervous System & Stress Reset
Stress dysregulates hormones and weakens immunity. Most people with lichen planus report flares during stressful times or unresolved trauma.
We teach practices to regulate your nervous system, from vagus nerve stimulation to somatic movement and breathwork. These reset your stress response and rewire how your immune system reacts.
A calm nervous system promotes hormonal balance and stops the immune system from attacking healthy tissues.
Lifestyle Changes That Support Healing

Healing from lichen planus requires more than taking pills — it requires a complete shift in how you nourish, move, and care for your body on a daily basis. This condition is often rooted in chronic inflammation, and addressing that inflammation holistically is key to long-term relief.
A clean, anti-inflammatory diet is foundational. Consuming nutrient-dense foods such as leafy greens, omega-3 rich fatty fish, turmeric, and gut-friendly fermented foods can help reduce systemic inflammation and support tissue repair. Removing inflammatory triggers like gluten, dairy, processed sugar, and artificial additives can drastically reduce flare-ups and support immune balance.
Movement is medicine — regular physical activity improves circulation, reduces stress hormones, and supports detoxification. Gentle exercises like walking, yoga, or tai chi are especially beneficial for calming the nervous system.
Sleep is when your body repairs. Prioritizing 7–9 hours of quality sleep each night helps regulate hormones and calm immune hyperactivity. Sleep hygiene practices such as turning off screens before bed, sticking to a sleep schedule, and avoiding stimulants late in the day are essential.
Finally, chronic stress is a major contributor to autoimmune flares. Integrating daily stress-reducing practices such as meditation, breathwork, journaling, or spending time in nature helps reset your nervous system and lower inflammation. Your lifestyle choices can either accelerate or resolve inflammation — and the power to choose lies in your hands.
The Role of Genetics and Epigenetics in Lichen Planus
- Genetic predisposition may increase your chances of developing autoimmune conditions such as lichen planus. If your parents or close relatives have autoimmune conditions, it can raise your risk. However, inheriting these genes doesn’t mean you’re destined to develop the condition.
- Functional medicine places a strong emphasis on epigenetics, which is the study of how your lifestyle choices — including the food you eat, how you manage stress, your sleep quality, and even your environment — can influence your genes. This means you have the ability to “turn off” genes that trigger autoimmune reactions.
- By modifying these lifestyle and environmental factors, you can actively shift your body’s internal state from inflammation to healing. This empowers you to take control of your health, rather than feeling helpless against your genetics.
- At Hormone Reset, we teach our clients how to use food, stress-reduction techniques, hormone balancing, and detoxification to influence gene expression and create an internal environment that no longer supports disease. Healing becomes not just possible — but inevitable with the right tools and guidance.
Ready to Finally Heal Your Skin — And What’s Beneath It?
You’ve tried the steroid creams, the mouthwashes, the endless guessing. But lichen planus isn’t just a skin issue — it’s your body asking for a reset.
At Hormone Reset, we don’t believe in band-aids. We believe in deep, lasting healing that starts from within.
This is your invitation to step into a new chapter — one where:
- Food no longer hurts your mouth
- Your skin feels calm, clear, and comfortable
- You wake up with energy and confidence
- You feel in control of your health again
Let’s uncover what your body’s been trying to tell you — and help you heal it at the root.
Conclusion: Healing Is Possible — And It Starts With You
Lichen planus may be an autoimmune condition, but it doesn’t define your future. It’s a sign — a message from your body that something deeper needs your attention and compassion. With the right guidance, the right tools, and the right mindset, you can reverse inflammation, restore balance, and reclaim the vibrant health you deserve.
At Hormone Reset, we’re here to walk that path with you — not just as practitioners, but as partners in your healing journey. Our functional medicine approach empowers you to heal not only your skin but your entire body, mind, and spirit.
You don’t have to live in fear of your next flare-up. You can feel at home in your body again. And it all begins with one choice: to go deeper, to heal smarter, and to believe that recovery is not just possible — it’s within reach.
References
- Lichen Planus: Symptoms and Causes – Mayo Clinic
https://www.mayoclinic.org/diseases-conditions/lichen-planus/symptoms-causes/syc-20351378 - Functional Medicine Approach to Autoimmune Diseases – iThriveIn
https://www.ithrivein.com/blog/functional-medicine-approach-to-autoimmune-diseases - Lichen Planus – Johns Hopkins Medicine
https://www.hopkinsmedicine.org/health/conditions-and-diseases/lichen-planus - Lichen Planus – NHS
https://www.nhs.uk/conditions/lichen-planus/ - Lichen Planus: Epidemiology, Clinical Features, Pathogenesis, and Treatment – NCBI Bookshelf
https://www.ncbi.nlm.nih.gov/books/NBK526126/
Review Article on Lichen Planus Pathogenesis and Treatment – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC11011293/